
Heel pain and plantar fasciitis
Heel pain and plantar fasciitis are the most common complaints seen in the podiatry office. As many sufferers know, heel pain can most certainly affect a patient's quality of life. A frequently diagnosed condition for those suffering from heel pain is plantar fasciitis. At this point you may be thinking "What is plantar fasciitis and how do I know if I have it?"
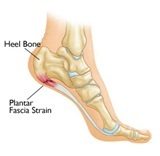
The plantar fascia is the flat band of tissue that connects the heel bone to the toes and supports the arch of the foot can become strained, weakened, swollen, and irritated. Heel pain (or fasciitis) is usually a sharp sticking pain in the bottom of the heel. This pain may radiate to the back or outside of the heel as well and can present with heel swelling. Most people with plantar fasciitis have pain when they take their first steps after getting out of bed in the morning or after sitting for extended periods of time.
Although plantar fasciitis is the most common cause of heel pain, heel pain can be caused by more than just plantar fasciitis. In most instances, heel pain or fasciitis is an overuse injury. However, sometimes heel pain is caused by bone injury, bone spur nerve injury, or irritation, muscle tightness, or neuropathy. As odd as they may seem some often overlooked causes of heel pain are low back injury, arthritis, or disc injury.

Why does heel pain happen?
Awkward landings (which may cause trauma erratic bone growth) or muscle strain are both things that can cause heel pain. These sources of heel pain, although agonizing, are less common. The most common source of heel pain can be thought of more as a repetitive motion injury. How we walk (our gait) and more importantly what we are wearing on our feet combine with life's daily activities to damage our heels and their structurally supportive network of tissue. The average person may feel a strain on the plantar fascia when they begin routinely performing a new activity or add on extra hours at work. Anything that keeps a person upright and on their feet for longer than normal can lead to this painful response.
Another major factor is shoes with poor support. Bare feet, soft soled shoes, or poor insoles (memory foam) usually aggravate the condition. The summer culprit - flip-flops - typically have poor support for the feet. Anyone who has spent a few hours walking or standing for too long in their flip flops has a story to share of the heel or foot discomfort symptoms mentioned above. Fortunately, many flip-flop manufacturers are beginning to create better supporting footwear. In general, a thinner and flatter shoe is going to put more tension and stretch on the plantar fascia potentially leading to plantar fasciitis.
What can be done?
X-rays are the first imaging test to be performed for heel pain and plantar fasciitis. This is to rule out any potential heel bone-based trauma and to narrow down the diagnosis to the probable cause. Over 90% of the time the treatment for fasciitis is a conservative approach; meaning that it very rarely requires surgery. Supportive shoes or a smaller heel on shoes will usually improve symptoms. From there, the treatment can range from taping, shoe gear, injections, shoe inserts, or many more options. In rare cases, fasciitis can be resistant to treatment and may require increased visits or surgery. In these extremely rare cases an MRI may be used to diagnose and treat resistant cases to rule out any obscure cause.
The biggest difference in getting the patient back on his or her feet is the podiatrist. Our podiatrists will develop and tailor a plan that works for you. When needed, Reid Podiatry will use the newest 3D digital scanner to make the appropriate shoe inserts for your condition. This scanning technology eliminates the many pitfalls of plaster casting and keeps the entire process in the hands of the physician.
You don't have to live in pain anymore let the staff at Reid Podiatry save your soles.

